How and Why Do Doctors Determine the Severity of Traumatic Brain Injuries?
How and Why Do Doctors Determine the Severity of Traumatic Brain Injuries?
Learn how medical professionals classify traumatic brain injuries to guide treatment, recovery, and support.
Request our Free Book on Traumatic Brain Injury

Understanding the different classifications of traumatic brain injury can help patients and their families anticipate the types of treatment and ongoing support they may need, leading to better outcomes for all of those affected by this often life-changing diagnosis.
In order to make an accurate diagnosis and TBI classification, medical practitioners take into consideration the severity of the injury, the patient’s symptoms, and the results of all testing and imaging, including CT scans.
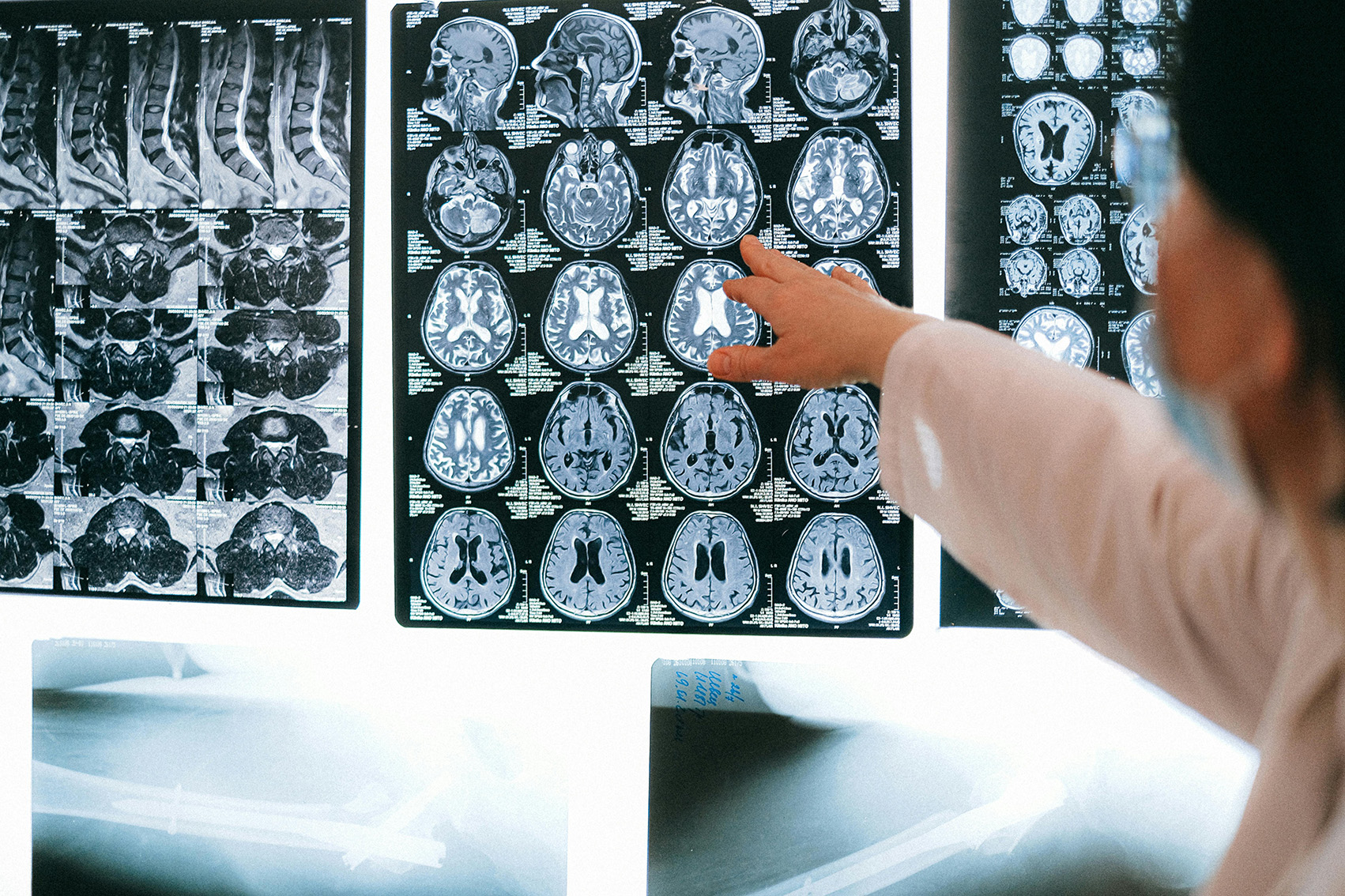
The Most Common Classifications for TBI
Mild traumatic brain injury (often referred to as a concussion) is the most common type of TBI. Concussions typically result in disruption of brain function, with symptoms such as:
- Confusion
- Headache
- Dizziness
Many individuals recover fully from a concussion within a few days to weeks, but in some cases, persistent lifelong symptoms may follow, and when this happens, it is known as post-concussive syndrome (PCS).
Moderate brain injuries involve considerable damage to the brain tissue, leading to more pronounced symptoms, such as:
- Prolonged loss of consciousness
- Memory loss
- Cognitive impairments
In these cases, rehabilitation is necessary to address residual deficits and promote recovery.
Severe traumatic brain injury involves extensive brain damage, resulting in long-term impairments in cognitive, physical, and emotional functioning. Individuals with severe TBI require intensive medical care, life-long rehabilitation, and support services to maximize their recovery and quality of life.
Sources: Mayo Clinic and Cincinnati Children’s Hospital Medical Center
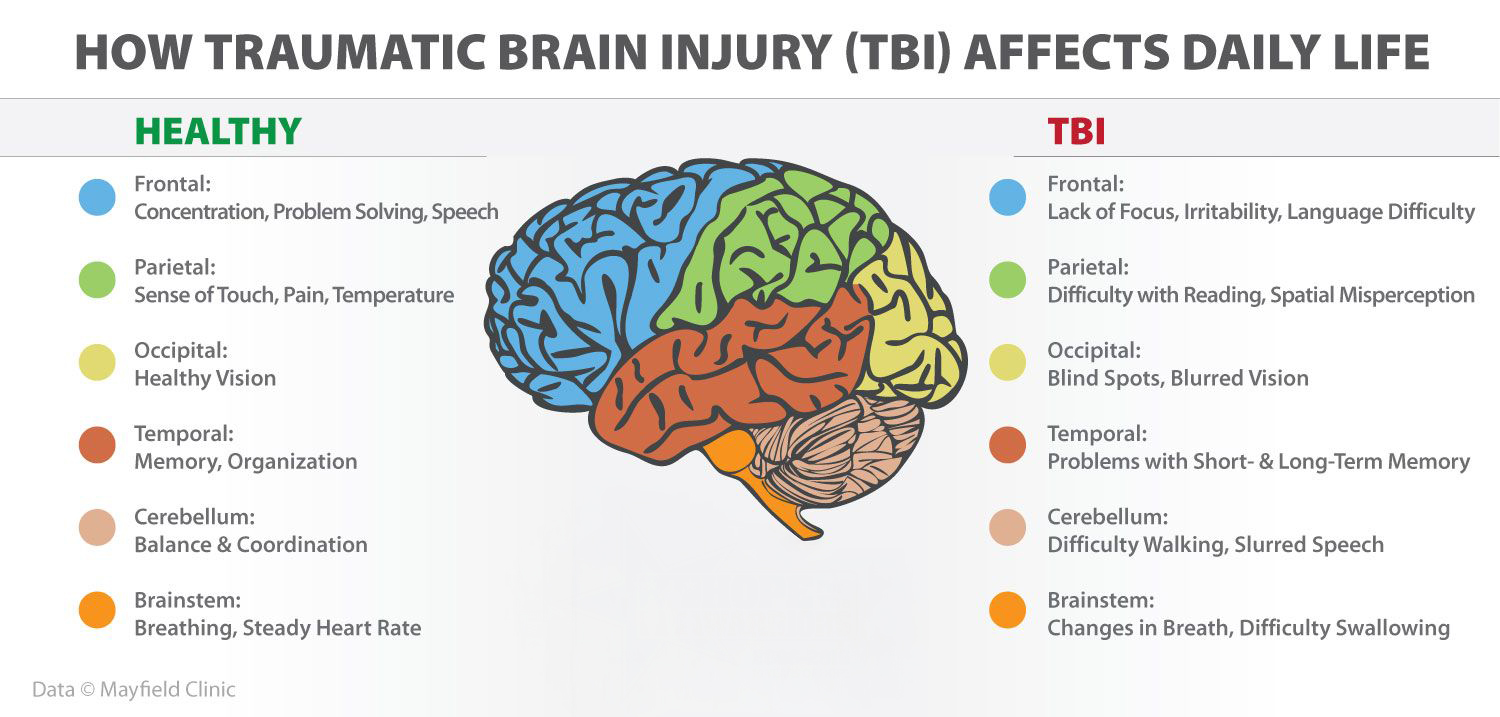
Why a “Mild” Brain Injury Can Still Be Serious
The word “mild” in a medical diagnosis can be deeply misleading — and when it comes to traumatic brain injury, it can give patients and families a dangerously false sense of security. In this clip, Stewart L. Cohen of Cohen, Placitella & Roth explores this critical issue with Dr. Thomas Swirsky-Sacchetti, a nationally recognized neuropsychologist.
Dr. Thomas Swirsky-Sacchetti: When people hear the term “mild,” they assume it’s not serious. And that’s one of the things I don’t like about the classification system — mild, moderate, and severe — because “mild” can actually be broken down further into complicated and uncomplicated.
A mild, uncomplicated head injury would be one in which there are no physiological markers — no skull fracture, no bleeding on the brain, no hematoma. A mild, complicated head injury — you can still have a skull fracture and bleeding on the brain, and it can still be technically classified as a mild head injury.
I saw one person — an older patient — who fell and didn’t even really lose consciousness. They had just a brief alteration of awareness, a little fuzzy for a few minutes. Their Glasgow Coma Scale score was near-perfect. They were classified as a mild head injury.
Six months later, they showed up in the emergency room because they had a slow bleed from that fall — a bleed that wasn’t picked up by the CT scan at the time because it had just started. But over six months, it grew to the size of a lemon. Their life was threatened. They wound up in emergency surgery with a neurosurgeon.
And that’s classified as a mild head injury.
Key Facts
2.5 Million
Approximate number of people who suffer a TBI each year
50,000
Result in death
80,000
Result in permanent disability
28%
Traumatic brain injuries are caused by accidents and falls
Keep in mind that the definitions of the types of TBI are broad and general and do not always help to explain the functional effect of a TBI on an individual patient. A patient with a so-called mild TBI — and their loved ones — can face a lifetime of consequences after the injury, including limitations on their ability to earn a living and their independence. Mild is a relative word, and the consequences of the injury can depend upon the perspective. No word or phrase is adequate to describe the cruel circumstances of a patient with a TBI diagnosis. Patients are not their labels. They are individuals who have suffered TBIs. Their injuries are unique, and they each travel on a very personal journey.
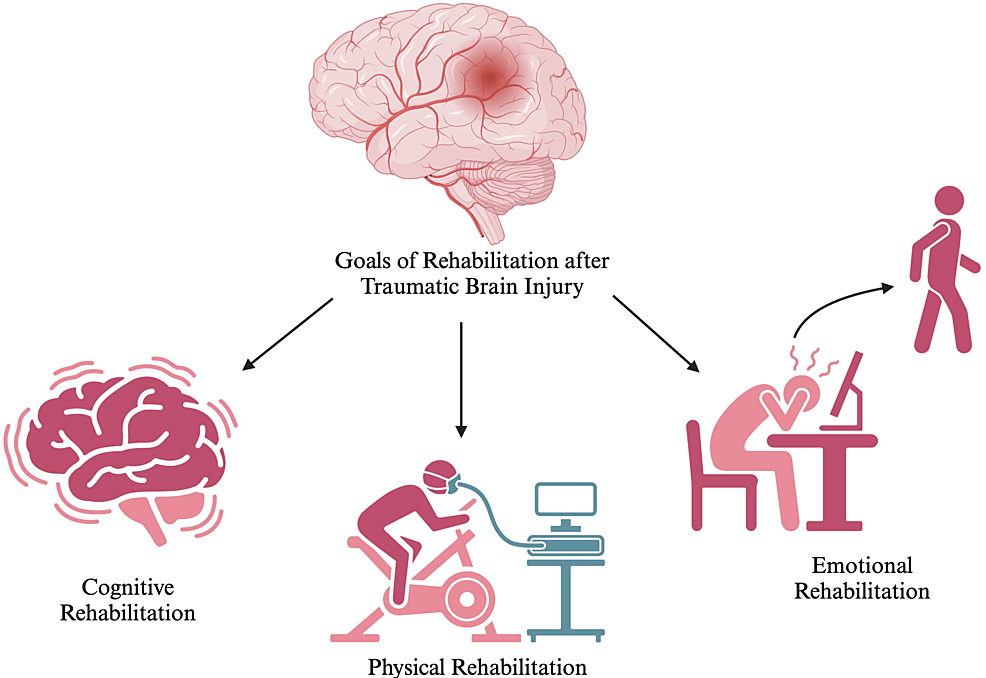
No matter the classification of a TBI, the effective management of the condition requires an appropriate and early diagnosis, targeted interventions, and comprehensive interdisciplinary care.
Why Don’t Brain Injuries Always Show Up on MRI or CT Scans?
In the clip below, Stewart L. Cohen of Cohen, Placitella & Roth discusses this issue in depth with Dr. Thomas Swirsky-Sacchetti, a nationally recognized neuropsychologist.
Stewart Cohen: In your experience, and based on your testing — do MRIs and CT scans always show the damage to the brain?|
Dr. Thomas Swirsky-Sacchetti: No. The rule of thumb is that an MRI — something has to be at least the size of your pinky fingernail in order for an MRI to pick it up. And sometimes, because they’re taking slices, if the lesion falls in between a slice, it can be missed. It’s less likely to be missed with repeated MRI.
But the problem with brain injuries is that the injury is on a microscopic level — it’s on a cellular level. So if you think about brain cells — they’re called neurons. There’s the cell body, and the axon, and then there are dendrites that come out. They don’t totally connect with the next neuron. There’s a space in between, and that’s where neurotransmitters come in.
Neurotransmitters are chemical bridges that allow electrical stimulation to travel down one neuron and jump that gap to stimulate the next neuron. So when you’re doing something like remembering a phone number, probably 50,000 of these neurons are firing in a second.
What happens in a head injury is that these neurons get twisted and pulled apart. So now the gap — the synapse — between the neurons is too big for those chemical bridges to work. And that’s why you have slower information processing. That’s why you have people who can’t find the right word to express themselves — it’s sort of reaching a dead end.
The other thing that an MRI or CT scan may not pick up is micro-hemorrhages — when tiny blood vessels, the capillaries, get broken. The skull is not a smooth surface on the inside — there are small bony protrusions, and when the brain gets shaken back and forth, it rubs against those protrusions, causing capillaries to break.
If it’s a major blood vessel, you’re going to find a collection of blood that’s visible on an MRI. But if it’s minor, as it often is, it won’t be. That’s why I tell people all the time to think about it in terms of structure and function — they’re not the same things.
Conversely, I’ve had people with huge, slow growing brain tumors that would basically wipe out their left frontal lobe – the size of a lemon. And on my testing I couldn’t find any functional impairment because the guy was really bright and this brain tumor was a slow-growing type. It might have been growing for 15 years. And it allowed him, because it was slow-growing, to begin to use his left frontal lobe to do things that the left frontal lobe would normally do. So yes, structure and function are two different things.
Gain a deeper understanding of the types, causes, symptoms, and treatments of each TBI classification by reading What Is Traumatic Brain Injury?
Need help investigating your legal rights related to a TBI?
Speak to an experienced brain injury attorney team like Cohen, Placitella & Roth.
For five decades, CPR has successfully represented individuals and families in TBI cases nationwide working with qualified co-counsel.


Get Our Free Traumatic Brain Injury Book
To learn more about Traumatic Brain Injury request our comprehensive book, available for free directly to your inbox




